Nephron
MCAT Biology
- Home
- »
- MCAT Masterclass
- »
- Biological and Biochemical Foundations of Living Systems
- »
- Biology
- »
- Nephron – MCAT Biology
Sample MCAT Question: Nephron
b) High salt permeability, low water permeability
c) High water permeability, low salt permeability
d) Low water permeability, low salt permeability
C is correct. High water permeability, low salt permeability.
The loop of Henle is a critical structure within the renal tubule that helps concentrate the urine. It consists of two parts, a descending limb and an ascending limb. The fluid that goes into the descending limb of the loop of Henle comes from the proximal convoluted tubule, and at this point, it is highly isotonic. The descending limb, however, has a high permeability to water and a low permeability to ions and urea. Furthermore, the fluid-filled space between the kidney tubules and the kidney medulla, or the interstitium, is highly concentrated. Therefore, as the isotonic fluid moves down the loop of Henle into the kidney medulla, water is reabsorbed into the kidney interstitium, and the fluid inside the tubules becomes highly concentrated.
Get 1-on-1 MCAT Tutoring From a Specialist
With MCAT tutoring from MedSchoolCoach, we are committed to help you prepare, excel, and optimize your ideal score on the MCAT exam.
For each student we work with, we learn about their learning style, content knowledge, and goals. We match them with the most suitable tutor and conduct online sessions that make them feel as if they are in the classroom. Each session is recorded, plus with access to whiteboard notes. We focus on high-yield topics if you’re pressed for time. If you have more time or high-score goals, we meticulously cover the entire MCAT syllabus.
Nephron
The nephron is the functional unit of the kidneys. In adults, each kidney contains approximately 1 million nephrons. Figure 1 shows the different components of a nephron. At the far left of the nephron diagram is the renal corpuscle, which consists of the Bowman’s capsule and the glomerulus. Then, from left to right, there is the proximal convoluted tubule, the Loop of Henle, which has both a descending portion and ascending portion, the distal convoluted tubule, and lastly, the collecting duct. For the MCAT exam, it is important to understand the order and the function of each of these nephron components in the production of urine.
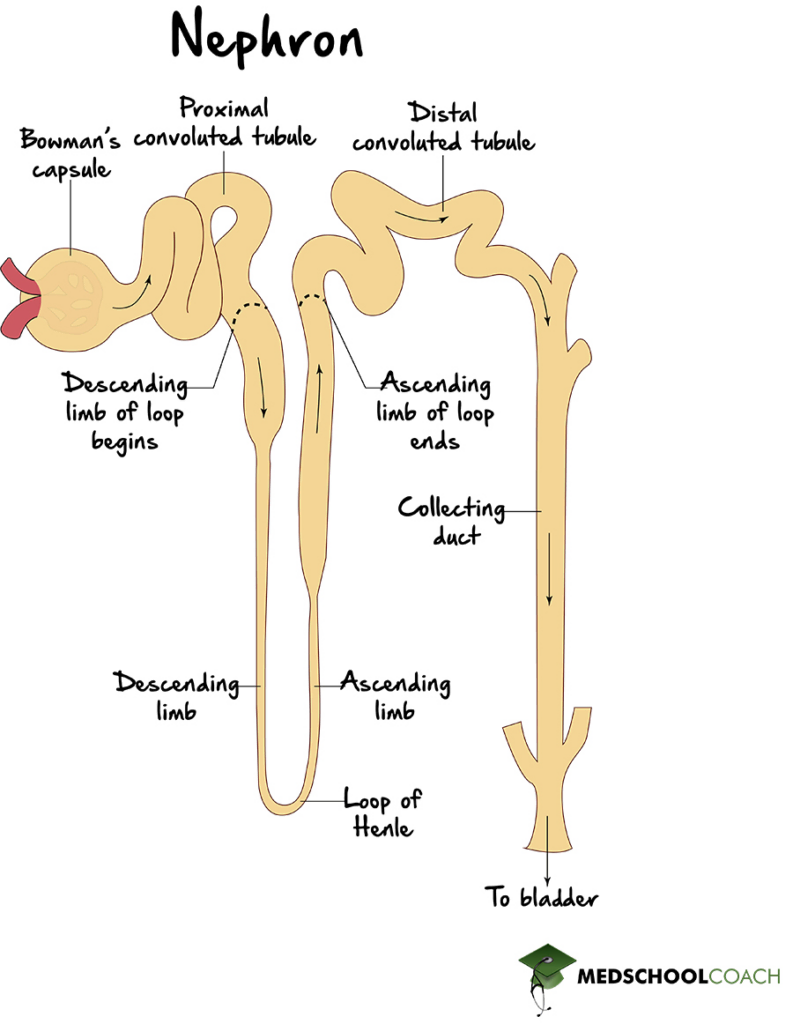
Bowman's Capsule
First, let’s look at Bowman’s capsule, where glomerular filtration occurs. Inside of the Bowman’s capsule are the glomerular capillaries, also referred to as the glomerulus. Recall that capillaries are the site of nutrient and waste exchange. In nephrons, this exchange is called glomerular filtration. Due to the high hydrostatic pressure of the fluid in the glomerular capillaries and the low solute concentration in Bowman’s space, fluid is forced across the glomerulus, into Bowman’s space, and, ultimately, into the renal tubule. This fluid is called ultra-filtrate. The ultra-filtrate consists of water and small solutes, and usually should not contain proteins or blood cells. Finding protein or blood cells in the urine is a sign of kidney damage.
Proximal Convoluted Tubule
From Bowman’s capsule, the filtrate passes into the proximal convoluted tubule (PCT). In the PCT, bulk reabsorption takes place, referring to reabsorption of the filtered blood. This reabsorption is not under hormonal control, and is called bulk reabsorption because approximately 70% of the fluid and solutes initially filtered into the renal tubule gets reabsorbed. The purpose of bulk reabsorption is to reabsorb solutes the body wants to keep, such as most of the glucose and amino acids that were filtered into the nephron in the first place.
Descending Limb of the Loop of Henle
From the PCT, the filtrate passes into the loop of Henle. The loop of Henle consists of multiple parts. The first part is called the descending limb of the loop of Henle. In the descending limb, the renal tubule has high water permeability and low salt permeability. And, because the concentration of the kidney tissue surrounding the tubule increases from the cortex to the medulla, as the filtrate passes down the descending loop of Henle, water moves out of the nephron and the solute concentration of the filtrate increases.
Ascending Limb of the Loop of Henle
From the descending limb of the loop of Henle, fluid moves into the ascending limb of the loop of Henle. The ascending limb of the Loop of Henle can be separated into the thin ascending limb, followed by the thick ascending limb. The thin ascending limb is impermeable to water and highly permeable to salt. Therefore, as the fluid moves up the ascending limb, the solute concentration in the tubule decreases as salt moves out of the thin ascending limb due to osmotic pressure.
The thick ascending limb, like the thin ascending limb, is also water impermeable. The difference between the two is that instead of salt moving out by moving out due to diffusion down its concentration gradient, there is active transport of solutes out of the thick ascending limb. This active transport is accomplished by the Na+-K+-2Cl– cotransporter, which will pump sodium, potassium, and chloride out of the renal tubule. The activity of this cotransporter is called the single effect and it’s important for the process of countercurrent multiplication, which produces the concentration gradient in the kidneys.
Distal Convoluted Tubule
From the ascending limb of the loop of Henle, filtrate moves into the distal convoluted tubule (DCT). The DCT is where regulated reabsorption occurs, meaning this is where hormones that affect urine composition act. One hormone is aldosterone, which increases sodium reabsorption by increasing the activity of the sodium-potassium pump. At the same time, as sodium is being reabsorbed, potassium is secreted into the urine. Another hormone that acts at the DCT is parathyroid hormone or PTH. PTH acts to increase calcium reabsorption in the kidneys.
Collecting Duct
Lastly, filtrate moves into the collecting ducts of the kidneys. The collecting duct is where antidiuretic hormone (ADH) or vasopressin acts. ADH will increase the production of aquaporins, which are water channels. In this way, ADH allows for water reabsorption into the body.
Explore More MCAT Masterclass Chapters
Take a closer look at our entire MCAT Masterclass or explore our Biochemistry lessons below.

One-on-One Tutoring
Are you ready to take your MCAT performance to a whole new level? Work with our 99th-percentile MCAT tutors to boost your score by 12 points or more!
See if MCAT Tutoring can help me
Talk to our enrollment team about MCAT Tutoring

MCAT Go Audio Course
Engaging audio learning to take your MCAT learning on the go, any time, any where. You'll be on the way to a higher MCAT score no matter where you are. Listen to over 200+ lessons.
MCAT Practice Exams
Practice makes perfect! Our mock exams coupled with thorough explanations and in-depth analytics help students understand exactly where they stand.
MCAT Prep App
Access hundreds of MCAT videos to help you study and raise your exam score. Augment your learning with expert-created flashcards and a question banks.