The Menstrual Cycle
MCAT Biology - Chapter 7 - Section 8.3 - Organ Systems - Reproductive System
- Home
- »
- MCAT Masterclass
- »
- Biological and Biochemical Foundations of Living Systems
- »
- Biology
- »
- The Menstrual Cycle – MCAT Biology
Sample MCAT Question - Menstrual Cycle
In terms of the menstrual cycle, at what phase does progesterone peak?
a) Ovulation
b) Luteal phase
c) Menses
d) Follicular
B is correct. Luteal phase.
During the luteal phase, the levels of progesterone are at a peak point as the now ruptured follicle begins to secrete progesterone. At this point, progesterone is providing support for the endometrium for potential implantation by the blastocyst. During the follicular phase and ovulation, the levels of progesterone are relatively low. Ovulation is also more specifically characterized by a surge in LH (choice A is incorrect). Also, the withdrawal of progesterone causes menses (choice C is incorrect). Estrogen reaches its peak point during the follicular phase (choice D is incorrect).
Get 1-on-1 MCAT Tutoring From a Specialist
With MCAT tutoring from MedSchoolCoach, we are committed to help you prepare, excel, and optimize your ideal score on the MCAT exam.
For each student we work with, we learn about their learning style, content knowledge, and goals. We match them with the most suitable tutor and conduct online sessions that make them feel as if they are in the classroom. Each session is recorded, plus with access to whiteboard notes. We focus on high-yield topics if you’re pressed for time. If you have more time or high-score goals, we meticulously cover the entire MCAT syllabus.
Menstrual Cycle Intro
The menstrual cycle, also known as the female reproductive cycle, is a 28-day cycle that prepares females for pregnancy. It can be divided into three main phases: the follicular phase, the ovulatory phase, and the luteal phase.
The Follicular Phase
The first phase of the menstrual cycle, known as the follicular phase, consists of the first 13 days of the cycle. During this phase, follicle-stimulating hormone (FSH) and luteinizing hormone (LH) are released from the anterior pituitary, and they stimulate folliculogenesis, which is the maturation of the follicle. In response, the follicle will secrete estrogen, which will have a function in developing the endometrium. Figure 1 shows the effects of rising estrogen levels on the developing endometrium. Also, as the follicle is developing, the primary oocyte within the follicle will complete meiosis I to form the secondary oocyte.
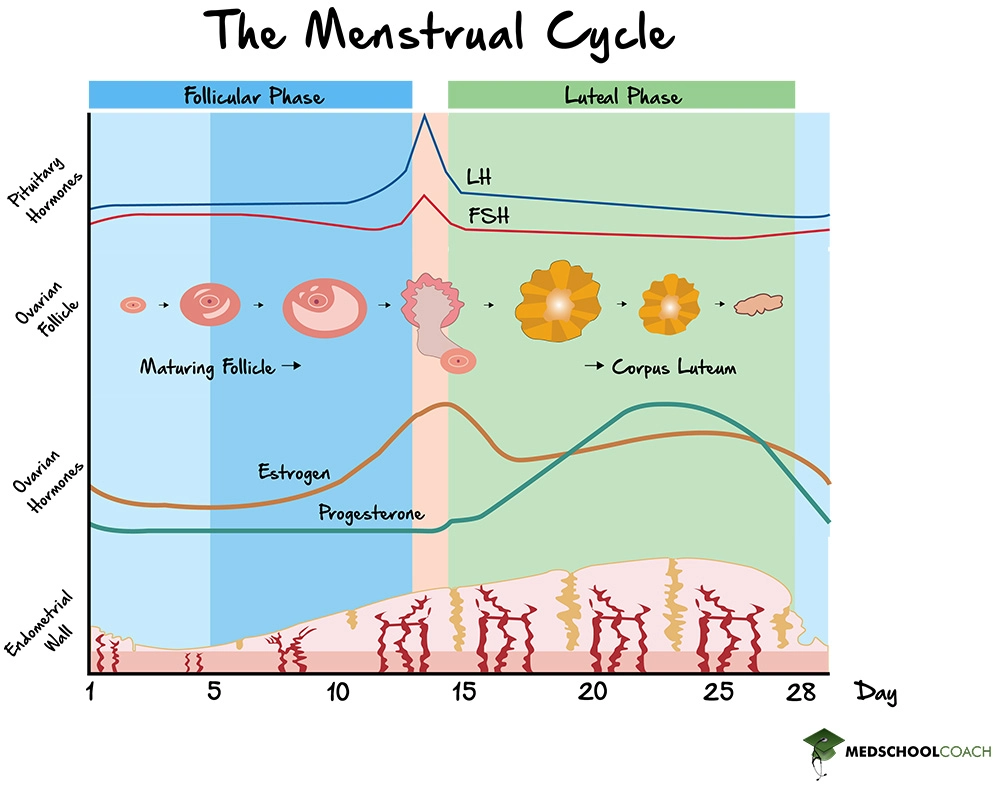
Furthermore, during the follicular phase, the effects of estrogen will change. At first, when the levels of estrogen are low, estrogen will have a negative feedback effect on the anterior pituitary gland, resulting in an inhibition of FSH and LH secretion. However, as the levels of estrogen gradually rise, they will reach a threshold. At this point, estrogen will have a positive feedback effect on the anterior pituitary. This effect causes a rapid surge in LH and FSH levels, which marks the start of the second phase of the female reproductive cycle, known as ovulation.
Ovulation
Ovulation in females is brought about by the spike in LH, called the LH surge. The LH surge starts at around day 12 of the menstrual cycle and can last up to 48 hours. The presence of LH matures the egg and weakens the wall of the follicle within the ovary. At some point, the fully developed follicle will rupture, resulting in the release of the secondary oocyte. At this point, the secondary oocyte can either be fertilized by a sperm cell or not. If not, the secondary oocyte will degenerate. Furthermore, since there are two ovaries, the one which ovulates occurs randomly. However, at times both ovaries can ovulate simultaneously, which may result in fraternal twins if both eggs are fertilized.
The Luteal Phase
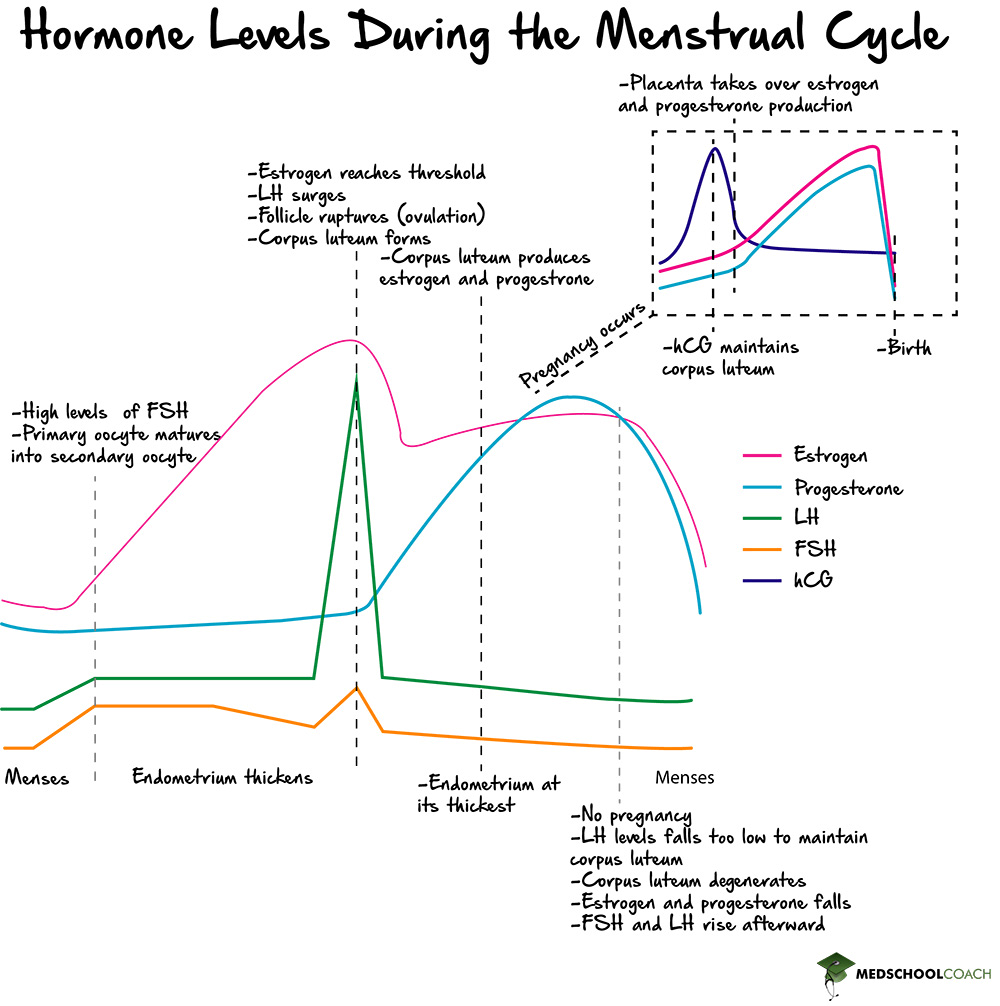
The remaining days of the menstrual cycle, from day 15 to 28, are known collectively as the luteal phase. The luteal phase is so named because the remaining follicle, without the secondary oocyte, forms what is called the corpus luteum. The corpus luteum secretes progesterone, which serves to further prepare the endometrium for implantation by the blastocyst. As Figure 2 shows, as progesterone is secreted, the endometrium becomes thicker and more vascularized. The progesterone is also essential for maintaining the endometrium as well.
If fertilization does not occur, the corpus luteum eventually degrades. When this happens, progesterone secretion stops, and soon after, the endometrium will be shed. Notice in Figure 2, how at the end of the luteal phase, the levels of progesterone drop, and the endometrium start the shedding process, also known as menstruation. As menstruation is finishing, it overlaps into the start of a brand-new follicular phase.
If, however, fertilization does occur, the process is different. Recall that fertilization involves the formation of a zygote from the fusion of an egg cell and a sperm cell. The zygote undergoes several developmental changes to form the blastocyst. The blastocyst is what implants into the endometrium, and this is known as implantation. When implanted, the blastocyst will begin to secrete human chorionic gonadotropin (HCG). HCG has an essential role in maintaining the corpus luteum, and while it is maintained, the corpus luteum will continue to secrete progesterone. The progesterone will, in turn, maintain the endometrium, so the blastocyst, after implantation, can develop.
Over time, the placenta will develop and take over the role of progesterone secretion from the corpus luteum. At this point, the rising HCG levels will drop, and also the corpus luteum will degrade. Meanwhile, the levels of estrogen and progesterone continually rise during the entire process.
Explore More MCAT Masterclass Chapters
Take a closer look at our entire MCAT Masterclass or explore our Biochemistry lessons below.

One-on-One Tutoring
Are you ready to take your MCAT performance to a whole new level? Work with our 99th-percentile MCAT tutors to boost your score by 12 points or more!
See if MCAT Tutoring can help me
Talk to our enrollment team about MCAT Tutoring

MCAT Go Audio Course
Engaging audio learning to take your MCAT learning on the go, any time, any where. You'll be on the way to a higher MCAT score no matter where you are. Listen to over 200+ lessons.
MCAT Practice Exams
Practice makes perfect! Our mock exams coupled with thorough explanations and in-depth analytics help students understand exactly where they stand.
MCAT Prep App
Access hundreds of MCAT videos to help you study and raise your exam score. Augment your learning with expert-created flashcards and a question banks.